
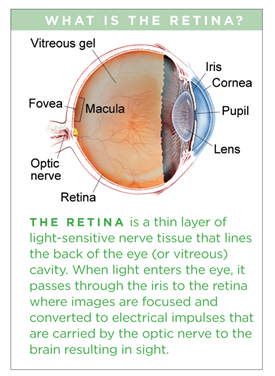
Retinal Tears
The retina is the inner lining of the eye; it is the thin, light-sensitive tissue that generates vision. Tears can form in the retina, creating a risk of retinal detachment and severe loss of vision.
PDF Fact Sheet Large-Print Version Spanish Translation Chinese Translation
Symptoms
A patient with an acute retinal tear may experience the sudden onset of black spots or “floaters” in the affected eye. This can have the appearance of someone shaking pepper in your vision. Flashes of light (Photopsia) are another common symptom.
If there is associated vitreous hemorrhage (bleeding in the clear cavity of the eye) or retinal detachment, additional symptoms can include blurred vision or a shadow as if curtains are closing in from the peripheral (side) vision. However, in some cases, a retinal tear may not manifest any noticeable symptoms.
Causes
The vitreous is a clear gel-like substance that fills in the back cavity of the eye which is lined by the retina. At birth, this gel is attached to the retina, but as we age, the gel separates from the retina creating a posterior vitreous detachment or PVD. In most cases, this happens without any issue.
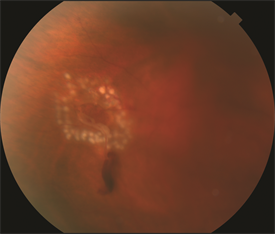
Figure 1. Laser photocoagulation around retinal tear with small hemorrhage. Photo courtesy of Larry Halperin, MD
However, in people who have an inherently more “sticky” vitreous, as the vitreous separates from the retina, it pulls abnormally (abnormal vitreo-retinal adhesion) and causes the retina to tear. Although retinal tears may also occur as a result of eye trauma, most retinal tears occur spontaneously due to a PVD.
A related entity are retinal holes. The term retinal tears and holes may be used interchangeably by some retina specialists. Retinal tears develop when the vitreous pulls on the retina while retinal holes develop due to progressive thinning of the retina. Retinal holes are typically smaller and have a lower risk for causing a retinal detachment. There are some instances where retinal holes should be treated the same as retinal tears.
Risk factors
Risk factors are not required to develop a retinal tear, but they make the likelihood greater. These factors include:
- Advanced age
- Degree of myopia (nearsightedness)
- Associated lattice degeneration (thin patches in the retina)
- Trauma
- Family history of retinal tears or detachment
- Prior eye surgery
There is no way to predict who might develop a retinal tear or when it might occur.
Diagnostic testing
A thorough and timely examination by a retina specialist using scleral depression (applying slight pressure to the eye) and/or a 3-mirror lens is the most important step in diagnosing a retinal tear. In cases where there is a limited view of the retina due to overlying hemorrhage, ophthalmic ultrasound may be required to aid in diagnosing a retinal tear.
Treatment and prognosis
If a retinal tear is diagnosed promptly before it progresses to retinal detachment, the prognosis is extremely good. Retinal tears are typically treated with laser or a freezing procedure (cryotherapy). Treatment is performed in an office setting and is very effective and quite safe.
Topical or local anesthesia is utilized, and the procedure is only mildly uncomfortable. The treatment creates spot-welding around the edges of the tear that nearly eliminates the risk of the tear progressing to retinal detachment. After a tear has been treated, there remains a future risk of developing additional, separate retinal tears; therefore, continued monitoring is important.
Not all retinal tears require treatment. When low-risk tears are identified in patients who have no symptoms, these tears can be observed without treatment. Some tears “treat themselves,” meaning they develop adhesion around the tear without treatment, and these situations can be followed without treatment as well.
