
Age-Related Macular Degeneration—Wet Forms Including Macular Neovascularization
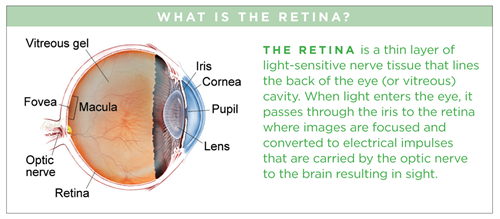
Age-Related Macular Degeneration (AMD) is a deterioration of the retina and choroid that leads to a substantial loss in visual acuity (sharpness of vision).
AMD is the leading cause of significant visual acuity loss in people over age 50 in developed countries.
Symptoms
In early stages, AMD may have no symptoms at all. When the disease progresses, the symptoms are:
- Distortion (warping) of straight lines
- A decrease in the intensity or brightness of colors
As the macular degeneration progresses, AMD symptoms include:
- A gradual or sudden loss of central vision, or
- Dark, blurry areas in the center of vision
Causes
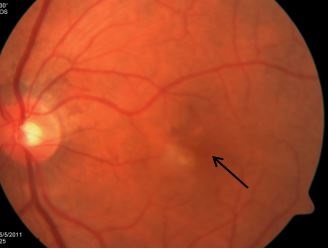
The exact cause of AMD is unknown, but the condition develops as the eye ages. There are 2 types of AMD: non-neovascular AMD or dry AMD; and neovascular AMD or wet AMD.
Macular Neovascularization (MNV) otherwise known as choroidal neovascularization occurs when abnormal blood vessels grow beneath the central part of the retina known as the macula, which is responsible for the sharp vision needed for reading and recognizing faces. These vessels can bleed or leak and cause a distortion of the retina’s structure. Ultimately, the MNV can turn into a disciform scar that replaces the normal architecture of the outer retina and leads to permanent loss of central vision. (Figure 1)
Risk factors
Risk Factors:
- Age—the strongest risk factor
- Family history of AMD
- Caucasian race
- Cigarette smoking
Possible risk factors:
- Female gender
- High cholesterol
- Lower level of education
- Sunlight exposure
- Light iris color
- Low dietary fish intake
- Far-sightedness
- Higher body mass index (BMI)
- Cardiovascular (heart) disease
- Having a diet low in lutein and
- High blood pressure zeaxanthin/antioxidants
Diagnostic testing
Disease features related to wet AMD may be found in the retina and in the layers beneath it.
A wet AMD diagnosis is made by a clinical examination with a slit lamp and by using several types of imaging, including:
- Fluorescein angiography (FA)
- Indocyanine green angiography (ICGA)
- Optical coherence tomography (OCT)
- Optical coherence tomography angiography (OCTA)
Treatment and prognosis
Wet-AMD treatment has been revolutionized in recent years after the discovery of vascular endothelial growth factor (VEGF), a family of compounds in the body. VEGF promotes the growth of abnormal new blood vessels in the eye—known as neovascularization—that can lead to wet AMD.
Anti-VEGF drugs have been developed to help control neovascularization and preserve vision for AMD patients. There are currently 5 available anti- VEGF drugs, athough more may be approved in the next few years
- Avastin® (bevacizumab)
- Lucentis® (ranibizumab)
- Eylea® (aflibercept)
- Beovu® (brolucizumab)
- Vabysmo® (faricimab)
Wet AMD cannot be cured, but its progression may be blocked with the use of intravitreal (in-the-eye) anti-VEGF injections. These injections may preserve, and even recover, vision. Local anesthetic eye drops are given before the injections to numb the eye and minimize discomfort.
There are 3 anti-VEGF treatment regimens commonly used for Avastin, Lucentis, Eylea, Beovu and Vabysmo. The best option is chosen in consultation with your retina specialist.
- Pro re nata (PRN) (As needed) or “treat and observe”—patients are treated with three initial monthly injections, followed by treatment as needed.
- “Treat and extend”—after 3 initial monthly injections, the time between treatments is gradually increased as long as the MNV does not show increased activity until a safe treatment interval is determined. Some eyes will continue to require monthly injections, but others can be treated less often as long as the wet AMD is controlled. Some patients may require treatment only every 10-16 weeks, depending on their response.
- Monthly injections. The anti-VEGF drugs are typically started with monthly injections, although this treatment regimen is used less often now with the extended duration of some anti-VEGF drugs.
Before the first anti-VEGF drugs were introduced, wet-AMD patients were treated with laser photocoagulation or photodynamic therapy (PDT), although these are used much less often now. There are occasional circumstances where these treatments are still used for the treatment of MNV.
Anti-VEGF drugs have greatly improved wet-AMD treatment since 2005; patients today have a much better chance of maintaining their central vision so they can read, drive, recognize faces, and live normal lives.
Although patients with wet AMD can experience a progressive decrease in visual acuity, they will almost never be completely blind.
